
Revolutionizing Respiratory Health: Reducing ED Visits and Hospital Readmissions with Nightingale Virtual Care
Executive Summary
Asthma and Chronic Obstructive Pulmonary Disease (COPD) represent two of the most common respiratory diseases. Together, over 40 million Americans suffer from asthma or COPD. While asthma affects all ages, COPD impacts mostly adults; however, each of these conditions is associated with exacerbations that are debilitating and require significant healthcare utilization. In the United States, the annual healthcare costs related to these complex diseases exceed $100 billion, largely due to repeated hospitalizations and emergency department (ED) visits from exacerbations.
Nightingale Virtual Respiratory Care by Health Care Originals offers a transformative solution for health plans and employers grappling with the high costs and care challenges associated with Asthma and COPD. Nightingale’s three-pronged technology-driven approach reduces these episodes by enabling better patient self-management and timely interventions. For health plans, this means lower claims and improved patient satisfaction; for employers, a healthier, more present workforce. Nightingale has succeeded in not only improving patient health outcomes but also in delivering economic benefits to partners in healthcare and industry.
Introduction
Clinical exacerbations from asthma or COPD are acute episodes where symptoms worsen significantly, necessitating immediate medical attention. Such exacerbations are a primary cause of emergency department (ED) visits and hospital readmissions, leading to increased direct and indirect costs due to the need for urgent intervention and subsequent care. As healthcare providers and payers seek to manage these diseases more effectively, the focus is shifting towards innovative care solutions that address the patients’ needs in their own homes. Despite the advancements in home-based and virtual care, optimizing these services to effectively reduce ED visits and readmissions remains an ongoing pursuit.
The Asthma and Allergy Foundation of America (2023) reports that about 40% of adults with asthma, and a higher percentage of children, experience at least one asthma attack per year. For individuals with COPD, Donaldson & Wedzicha (2006) highlight that exacerbations increase with the disease’s severity, with approximately 20% of patients enduring almost three exacerbations annually, emphasizing the urgent need for effective management strategies to mitigate these critical events.
Healthcare Utilization Outcomes
For health plans and employers, the management of Asthma and COPD is a significant concern due to the substantial healthcare utilization these conditions necessitate, particularly in terms of hospitalizations, emergency department (ED) visits, and readmission rates. Exacerbations of these diseases not only lead to increased healthcare service use but also contribute to the high direct costs associated with managing respiratory conditions.
Data from 2019 indicates that the rate of ED visits for individuals with asthma was 108.4 per 10,000 for children and 41.8 for adults, whereas COPD-related ED visits were at 40.2 per 10,000 individuals, amounting to more than 1.3 million visits (American Lung Association, 2023; Center for Disease Control and Prevention, 2020). The National Hospital Ambulatory Medical Care Survey further underscores the burden of these conditions, reporting that asthma and COPD accounted for 9.7% and 6.3% of all ED visits in the United States in 2020 (National Center for Health Statistics, 2020).
Hospitalizations remain a critical metric, with reported rates of 5.2 and 16.3 hospital stays per 10,000 individuals for asthma and COPD, respectively. The Centers for Disease Control and Prevention (2022) noted over 169,330 inpatient stays and more than 1.8 million ED visits for asthma as a primary diagnosis in 2019.
Readmissions, particularly within 30 days of discharge, represent a costly and often preventable outcome. The Hospital Readmissions Reduction Program (HRRP) by CMS now includes COPD as a condition of focus due to its high readmission rates, which were reported at 22.6% for COPD and 11.9% for asthma (N. Patel et al., 2022; Shah et al., 2015). These rates are consistent with findings by Press et al. (2021), who noted nearly a 20% 30-day readmission rate for COPD.
For health plans and employers, these figures are alarming as the cost implications are significant. A systematic review by Bollmeier & Hartmann (2020) highlighted that the mean cost for treating a COPD exacerbation requiring hospitalization can range from $7,000 to $39,200. With healthcare costs expected to rise, hospitalizations and readmissions for exacerbations are the predominant cost drivers for these respiratory diseases, emphasizing the need for effective disease management strategies to control healthcare spending and improve outcomes for affected populations.
Chronic Respiratory Disease Management
Proper management of asthma and COPD is crucial for reducing ED visits and hospital readmissions. Strategies that combine effective medication, patient education, and early exacerbation detection have been shown to lessen hospital admissions (Bollmeier & Hartmann, 2020). Self-management education is also a key component in effective disease control, as highlighted by the CDC’s 6|18 initiative and the Global Initiative for Chronic Obstructive Lung Disease guidelines. Moreover, home-based care and tracking have been identified as effective in reducing readmission rates for COPD and hospital stays for asthma (Shelledy et al., 2009; Truumees et al., 2022), presenting a viable option for health plans and employers to consider in their healthcare strategies.
Virtual Care Programs
Health Care Originals’ Nightingale Virtual Respiratory Care delivers a comprehensive virtual care model aimed at enabling patients with respiratory diseases to achieve self-sufficiency in managing their conditions. Nightingale’s distinctive three-pronged approach integrates a wearable device (ADAMM-RSM), digital data analytics, and clinician support to form the core of its service.
The ADAMM-RSM wearable device is a standout element of Nightingale. This discreet, lightweight track captures a wide range of respiratory data, including the frequency and type of coughs, which is vital for managing asthma and COPD. Unlike other devices, ADAMM-RSM is adept at functioning in cases of chronic cough—a common and challenging aspect of respiratory disease management. Moreover, it records cough-induced body motions, positions, and provides time-stamped data for each cough, offering detailed insights to guide patient care. Beyond cough analysis, the device also tracks respiration rate, heart rate, temperature, and activity, providing real-time, quantitative data to both patients and healthcare providers.
Preliminary Results
Nightingale Virtual Respiratory Care has shown promising preliminary results in reducing disease-related impairment and symptoms for its members. With a median participant group of 74, Nightingale utilized the St. George’s Respiratory Questionnaire (SGRQ) to gauge health-related quality of life (HRQoL) and symptom severity over time.
As outlined in Figure 1, HRQoL scores improved from a baseline average of 44 to 24 at the three-month mark, indicating fewer limitations due to disease. This improvement was maintained over time, with a significant drop to 21 at the 12-month evaluation, corresponding to 60% of members demonstrating clinically meaningful improvements.
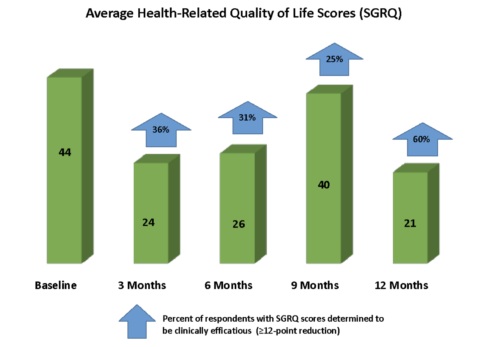
Figure 1. Average health-related quality of life (HRQoL) scores (SGRQ) reported by participants at baseline and over time enrolled in Nightingale (data provided by Health Care Originals, 2023).
Symptom scores also showed substantial reductions, with a decrease from 64 at baseline to 36 at the 12-month checkpoint (Figure 2). At six months, 63% of members reported clinically significant reductions in symptoms, and after 12 months, 50% maintained this improvement.
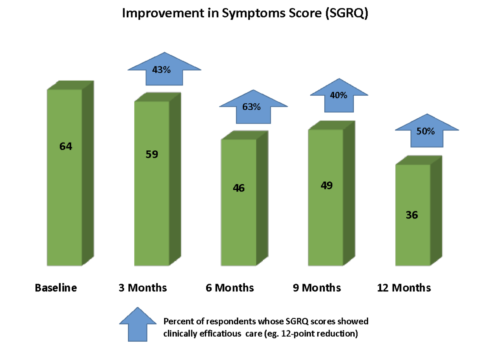
Figure 2. Average symptom scores (SGRQ) reported by participants at baseline and over time enrolled in Nightingale (data provided by Health Care Originals, 2023).
These positive trends in HRQoL and symptom scores suggest that Nightingale’s approach may contribute to decreased ED visits and hospital readmissions by effectively reducing the severity of disease symptoms and the overall impact on patients’ lives.
Discussion
Nightingale Virtual Respiratory Care by Health Care Originals has been effective in improving quality of life and symptom management for chronic respiratory patients. It also potentially reduces emergency department (ED) visits and hospital readmissions. This approach, effective for conditions like diabetes, is pertinent for health plans and employers impacted by healthcare costs.
Nightingale patients reported significant improvements in health-related quality of life and symptom scores, indicating better disease control. This likely contributes to reduced acute exacerbations leading to ED visits and readmissions. Despite a decrease in improvements at nine months due to seasonal exacerbations, sustained long-term benefits were observed over a year, suggesting lasting effects on reducing acute care utilization.
The preliminary data from Nightingale supports the viability of virtual care in reducing ED visits and hospital readmissions for chronic respiratory disease patients, offering a model for healthcare providers and payers focused on optimizing utilization outcomes.
Conclusions
Inadequate management of chronic respiratory diseases like COPD and asthma diminishes quality of life and burdens the healthcare system through increased hospital and ED utilization. Effective management is paramount for improving health outcomes and healthcare cost savings.
Health Care Originals (HCO) leads in virtual respiratory care with Nightingale, enhancing clinical outcomes and reducing healthcare utilization, including ED visits and hospital readmissions. This is achieved through tailored self-management education, continuous tracking with ADAMM-RSM technology, and support from healthcare professionals.
Nightingale’s personalized approach, combined with its scalable model, positions it as an innovative solution in managing chronic respiratory conditions, potentially transforming patient care and reducing economic impact on the healthcare system.


