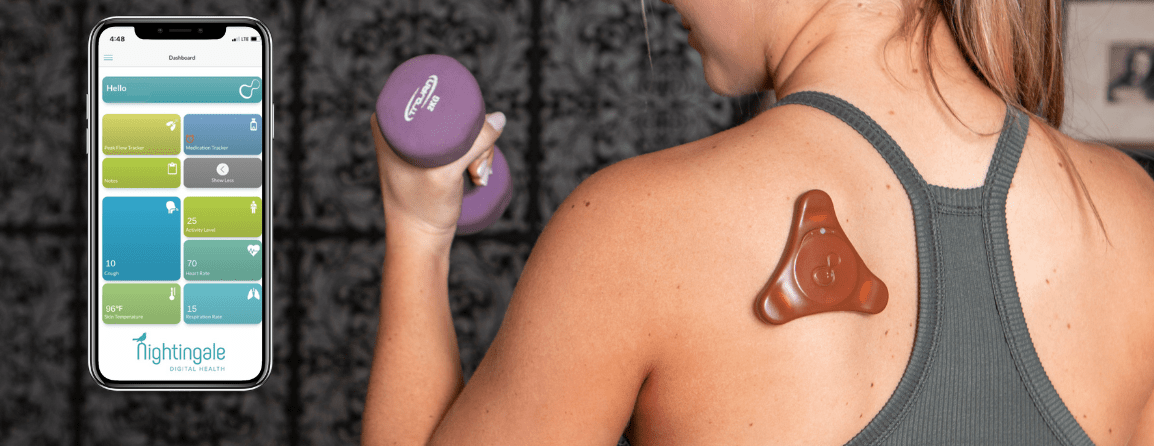
Digital biomarkers have revolutionized the landscape of clinical studies in various fields of medicine, including respiratory disease. These objective, quantifiable physiological and behavioral data points collected through digital devices have provided researchers and healthcare professionals with valuable insights into the progression and management of respiratory conditions. So, let’s dive into the fascinating history of digital biomarkers in clinical studies for respiratory disease, exploring the milestones and breakthroughs that have shaped this exciting field.
Incorporating Wireless, Wearable Technology, and Mobile Applications in Respiratory Clinical Studies
Wireless and Wearable Technology (Early 2000s)
The initial steps towards incorporating digital biomarkers into clinical studies for respiratory diseases began in the early 2000s with the advent of wireless and wearable technology. This new era of connected devices, such as pulse oximeters, spirometers, and activity tracks, enabled researchers to collect real-time data from patients, providing a more comprehensive understanding of disease progression and response to treatment.
The Impact of Mobile Applications (Mid-2000s)
In the mid-2000s, the increasing prevalence of smartphones and mobile applications opened up new avenues for collecting and analyzing digital biomarkers in respiratory disease. Mobile apps designed to track symptoms, medication adherence, and lung function became valuable tools for both patients and healthcare professionals. These advancements allowed for remote tracking and management of respiratory conditions, such as asthma and chronic obstructive pulmonary disease (COPD), leading to improved patient outcomes and reduced healthcare costs.
Wearable Devices and the Internet of Things (2010s)
As the 2010s rolled around, the field of digital biomarkers continued to expand, fueled by the growing interest in wearable technology and the Internet of Things (IoT). Wearable devices like smartwatches and fitness trackers began to offer features specifically designed for respiratory health tracking, such as heart rate variability analysis and respiration rate tracking. This wealth of data enabled researchers to study the relationship between physical activity, sleep patterns, and respiratory health, paving the way for personalized treatment strategies.
Leveraging Artificial Intelligence and Machine Learning
The rise of artificial intelligence (AI) and machine learning in the late 2010s further accelerated the growth of digital biomarkers in respiratory disease research. These advanced computational methods allowed researchers to analyze complex datasets, identifying subtle patterns and correlations that could not be detected using traditional statistical techniques. As a result, AI-driven algorithms have been developed to predict exacerbations in asthma and COPD patients, empowering healthcare providers to intervene early and prevent severe episodes.
The Role of Digital Biomarkers during the COVID-19 Pandemic
During the COVID-19 pandemic in the early 2020s, digital biomarkers played a crucial role in tracking and managing respiratory health on a global scale. Remote patient tracking systems and telehealth platforms enabled healthcare providers to assess patients’ respiratory status without exposing them to potential infection risks. Digital biomarkers collected through these technologies have helped track the progression of the disease, identify high-risk individuals, and evaluate the efficacy of various treatment options.
In summary, the history of digital biomarkers in clinical studies for respiratory disease is marked by continuous innovation and a commitment to improving patient care. From the early days of wireless technology to the current era of AI and IoT, digital biomarkers have reshaped the way respiratory diseases are studied, diagnosed, and treated. As we look to the future, there is no doubt that digital biomarkers will continue to play a vital role in advancing our understanding of respiratory disease and revolutionizing patient care.
How does ADAMM help? Also, how does ADAMM help make real-world evidence more feasible to collect?
ADAMM, which stands for Automated Device for Asthma Tracking and Management, is a wearable technology designed to assist in the early detection and management of asthma symptoms. Developed by Health Care Originals, ADAMM is a smart, discreet, and non-invasive device that can be worn on the upper torso. It helps both patients and healthcare providers by collecting real-time data on various physiological parameters, making real-world evidence more feasible to collect. Here’s how ADAMM contributes to asthma management and the collection of real-world evidence:
- Early detection of symptoms: ADAMM continuously tracks the user’s respiration rate, heart rate, and cough frequency, allowing for early detection of potential asthma flare-ups. The device can also recognize wheezing sounds, which are often indicative of airway obstruction. By identifying these symptoms early on, patients can seek timely medical intervention, improving their overall health outcomes.
- Personalized management: ADAMM is capable of tracking and recording medication usage, which helps patients and healthcare providers better understand the effectiveness of treatment plans. This data enables more personalized management of asthma, as healthcare providers can adjust medications based on individual responses and needs.
- Remote tracking and telehealth: The data collected by ADAMM can be accessed by healthcare providers remotely, enabling them to track their patients’ asthma status without the need for in-person visits. This not only reduces healthcare costs but also allows for more convenient and efficient management of asthma, especially in remote or underserved areas.
- Real-world evidence collection: ADAMM’s ability to continuously collect physiological data in real-life settings makes it an invaluable tool for generating real-world evidence. This data can be used to assess the effectiveness of asthma treatments, track disease progression, and identify triggers in patients’ daily lives. Real-world evidence is crucial for understanding the true impact of interventions and informing clinical practice and policy decisions.
- Patient engagement and education: ADAMM’s companion app provides patients with insights into their asthma management, helping them stay engaged in their care. The app offers personalized feedback, medication reminders, and trend analysis, empowering patients to take a more active role in managing their condition.
By providing continuous tracking, early symptom detection, personalized management, remote access, and real-world evidence collection, ADAMM helps improve asthma care and outcomes for patients. The technology’s ability to collect data in real-world settings greatly enhances our understanding of asthma and its management, ultimately benefiting both patients and healthcare providers.


